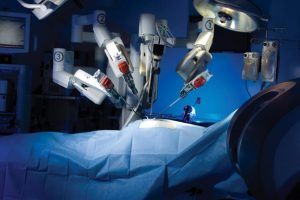
What is Robotic Surgery? The Precision Revolution in Modern Medicine
MEDTECH STRATEGIC INSIGHT – In the history of medical science, the leap from traditional open surgery to laparoscopy was a milestone. Today, we are witnessing an even greater evolution: the era of robotic-assisted surgery (RAS). Far from the science-fiction trope of “autonomous robots,” modern surgical robotics represents the ultimate synergy between human intuition and machine precision.
As of 2026, with the deployment of fifth-generation systems like the da Vinci 5 and the modular Hugo RAS, robotic surgery has become the gold standard for complex operations worldwide.
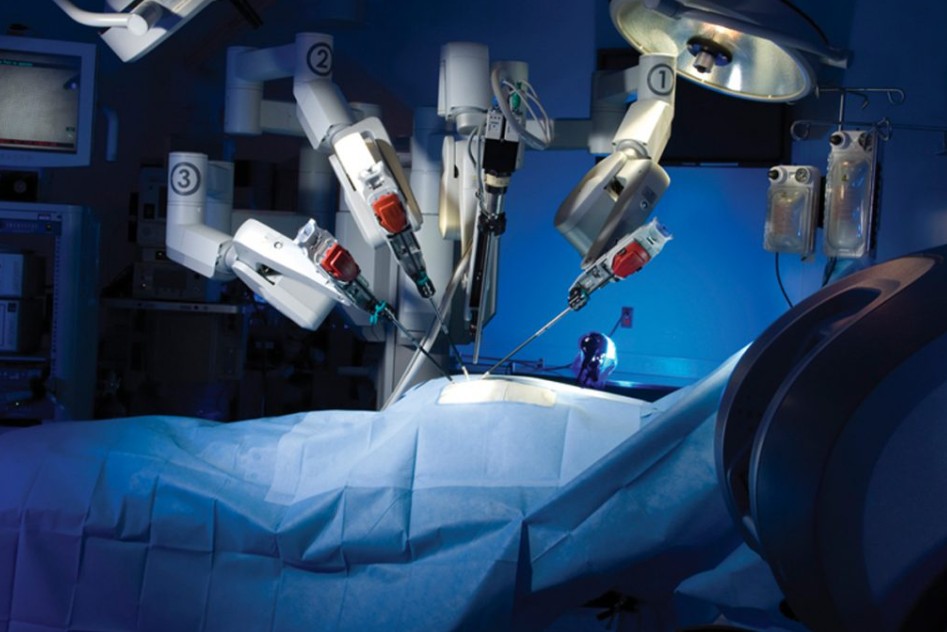
Understanding the Mechanism: How It Works
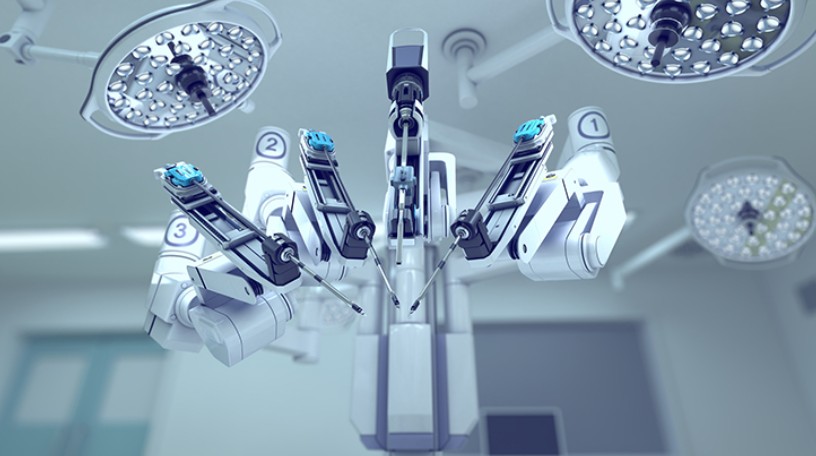
It is a common misconception that the robot performs the surgery. In reality, the robot is a sophisticated tool entirely controlled by a human surgeon. The system typically consists of three components:
-
The Surgeon Console: Where the lead surgeon sits and operates hand and foot controls while viewing a high-definition 3D image of the surgical site.
-
The Patient-Side Cart: The robotic arms that hold miniaturized instruments and a 3D camera.
-
The Vision System: Advanced software that translates the surgeon’s large hand movements into micro-movements inside the patient’s body.
The core technology behind this is Motion Scaling and Tremor Filtration. The system filters out the natural tremors of the human hand, allowing for a level of steadiness that was previously impossible.
Broad Horizons: Where is it Used?
Initially pioneered for urology, robotic surgery has rapidly expanded into almost every major surgical field:
-
Urology: Especially for prostate and kidney surgeries where nerves must be meticulously preserved.
-
Gynecology: Used for complex hysterectomies and endometriosis treatments.
-
General Surgery: Hernia repairs, colorectal cancer resections, and weight-loss surgeries.
-
Cardiothoracic Surgery: Performing heart valve repairs without the need for traditional “open-heart” chest incisions.
-
Orthopedics: Specialized systems like the Mako platform assist in ultra-precise hip and knee replacements.
The Strategic Advantages: Why Choose Robots?
The move toward robotic assistance is driven by measurable clinical outcomes. The benefits are dual-sided, impacting both the medical team and the patient.
For the Patient:
-
Smaller Incisions: Instead of a single large cut, surgeries are performed through tiny “keyhole” ports.
-
Minimal Blood Loss: Precision tools cauterize and cut with such accuracy that blood loss is significantly reduced.
-
Faster Recovery: Patients often return to their normal lives days or even weeks earlier than traditional methods.
-
Reduced Pain and Infection Risk: Smaller wounds mean less post-operative trauma and lower rates of surgical site infections.
For the Surgeon:
-
Superior Visualization: 3D HD views provide depth perception and magnification up to 10x, revealing details invisible to the naked eye.
-
Enhanced Dexterity: Robotic “wrists” can rotate 360 degrees—a range of motion far exceeding the human hand.
-
Ergonomics: Sitting at a console reduces physical fatigue during long, multi-hour procedures, ensuring peak performance from the start to the end of the operation.
The Future: AI and Telesurgery
As we look toward the late 2020s, the next frontier is the integration of Artificial Intelligence (AI). Future systems are being trained to provide “augmented reality” overlays, highlighting critical nerves or tumor margins in real-time. Furthermore, the development of low-latency 6G networks is making Telesurgery—a surgeon operating on a patient in another city or even a combat zone—a practical reality.
In the world of defense and tech, the advancement of surgical robotics is more than just a medical trend; it is the blueprint for the future of human-machine interaction.
Editor’s Note: This guide is based on 2026 clinical standards and the latest FDA-cleared platforms. Defense & Tech will continue to monitor the impact of AI-driven surgical robotics on global healthcare infrastructure.